Training Needs for Medical Science Liaisons (MSLs) in Evolving Pharmaceutical and MedTech Industries
Download the full article here
By
Ajit Patwardhan, MD1, MBA; Robin Winter-Sperry, MD2; Dannielle Heuer3; Stephen Valerio4; Urvashi Vashee5; Drilon Saliu, PharmD, MBA6; Greg Christopherson, PhD7; Irma Saliu, PharmD8; Kyle Kennedy9; Michelle Powell, PharmD10; Chris Brock, PharmD11 ; John B Pracyk, MD, PhD, MBA12; Joe Medicis, PharmD13
1 Physician – Surgeon, Medical Affairs Executive – Baxter International, Integra LifeSciences, NLT Spine, Paradigm Spine
2 President, Scientific Resilience; MAPS 2020 Co-Chair
3 Director WD Communications
4 Sr Director, Oncology Medical Training AstraZeneca
5 Global Scientific Training Merck & Co
6 Head, Global Medical Affairs, Clinical Development and HEOR, Connected Care Philips
7 VP, Medical Affairs Medline
8 National Director, Psychiatry MSLs, US Field Medical Allergan
9 VP, Customer Strategy – The Medical Affairs Company
10 Director, Filed Medical Excellence Astellas Medical Affairs Americas USA
11 Field Based Medical Affairs, Head, Respiratory GlaxoSmithKline
12 Integrated Leader, Medical Affairs, Pre-Clinical, & Clinical Research DePuy Synthes Spine, (J&J)
13 Director US Medical Affairs Callidiatas Therapeutics

ABSTRACT
The evolving role of Medical Sciences Liaisons (MSLs) was extensively discussed in multiple presentations and workshops at the March 2020 Medical Affairs Professional Society (MAPS) Global Annual Meeting in Miami, Florida. Executive leaders with domain expertise in building and managing Field Medical teams shared their experience and views on the value proposition of these roles and how a changing healthcare and industry landscape is influencing differentiation of and new opportunities for this role. The leaders also recognized the increased need for specialized training and how adult learning principles along with integration of new creative digital tools could help enhance engagement, performance and career growth. This article formalizes these learnings, providing best practices for MSLs in the context of the ongoing pandemic and beyond.
INTRODUCTION
MSLs represent a core function of Medical Affairs, acting as the medical face of the organization to provide deep sub-specialty knowledge to healthcare providers and other external stakeholders. MSLs’ primary responsibility focuses on the three pillars of Medical Affairs, i.e. Scientific Exchange, Evidence Generation, and Evidence Dissemination. As such, a primary function of the MSL role is to build and execute an engagement plan in an expanding thought-leadership network. Currently, both the development of these plans and the actions that allow MSLs to deliver on their promise are undergoing sea change.
Over the last decade, healthcare delivery has undergone sweeping reforms. Emerging trends now focus on substantially better cost, quality, and outcomes as the new parameters to demonstrate significant healthcare value. Patients are now at the center of making their healthcare decisions and are demanding data transparency, easy/convenient access, and personalized products and services. Increased need for data transparency and availability has given rise to disruptive technologies and technological advances in the form of advanced data analytics, artificial intelligence, machine learning, digitization, new social media platforms, etc. Alongside these societal and cultural changes, stricter regulations and adjustments to healthcare policy (e.g. changing insurance landscape, use of Real World Evidence, new European Union (EU) regulations, increased scrutiny on drug pricing and rebates, etc.) are driving new ways of thought and action in the healthcare landscape. Meanwhile, the promise of new technologies driving basic and translational research have led Pharmaceuticals and MedTech industries to renew their focus on R&D and scientific advances, leading to personalized medicine breakthroughs in drug-device combinations, small molecule therapeutics, biologics, immunotherapy and diagnostic biomarkers, regenerative medicine and many more areas of advancement in the life sciences industry.
With these dynamic changes taking place in the healthcare landscape, the traditional role of an MSL as a bridge between internal company stakeholders and the outside medical community now needs to expand to encompass new competitive skillsets focusing broadly on Products, People, Personal & Platforms (“4Ps”). The following description of these 4Ps is not meant to be comprehensive, but rather is an attempt to start a new conversation about these core areas to better equip MSLs with a forward-looking understanding of the skill sets needed to succeed in the current and future disrupted healthcare landscape.
PRODUCT
Due to increased need for personalized medicine (as described in part above), complex treatment options require deep therapeutic area expertise, which for MSLs includes the following:
- Understand the therapeutic area landscape and the complex treatment options
- Understand the clinical research and clinical practice specific to the therapeutic area
- Understand the patient journey and needs of patients in the patient-centric model of care
- Understand the marketplace including product competition and current/future scientific advances in the therapeutic landscape
- Understand the economic value of the drug or device in consideration, including current and future drug/device pricing along with improvement in clinical and quality of life functional outcomes
- Understand (and first generate) clinician and patient insights on current evidence needs and demands.
- Understand how to share these insights internally to support new indications, new target markets, and possible new clinical development approaches including RWE studies, investigator-initiated studies / research (IIS/IIRs), comparative effectiveness studies, etc.
PEOPLE
The model of proscriptive medicine in which treatment decisions were made almost solely by healthcare providers has given way to a new model in which patients are collaborators or even drivers of treatment choices, often taking into account quality of life alongside quantity of life. This shift results in new stakeholders, including but certainly not limited to the following:
- New patient populations based on personalized/individual disease traits, disease incidence, etiology, pathogenesis, clinical outcomes
- Integrated delivery networks (IDNs) & payors, market access and reimbursement groups, accountable care organizations (ACO’s), ambulatory surgery centers (ASC’s), patient advocacy groups, pharmacy & therapeutics committee (P&T), value analysis committee (VAC) with non-clinical leadership decision makers (e.g. supply chain, finance, quality, IT, peri-operative services, etc.)
- Digital KOLs, real-world physicians/surgeons and specialists, local/community HCPs (supported by community focused MSL teams i.e. Community Medical Liaisons)
PLATFORMS
Along with new Products and new People are new Platforms that offer significant opportunity for MSLs to reach stakeholders with new creative digital tools for scientific engagement and education, including the following:
- Public-facing and HCP-facing digital media including articles, podcasts, social media, virtual events, and even thought-leader forums such as TED talks and other curated communication events
- Emerging tools for data visualization and scientific knowledge exchange including advanced data analytics, artificial intelligence/machine learning, virtual and augmented reality. Of course, along with the ability to generate more data and increasingly granular data, MSLs are challenged to discover and utilize innovative ways to customize data for external and internal information consumers
- Virtual communication platforms, e.g. Zoom, WeChat, Salesforce, Google hangout, etc. These digital platforms allow MSLs to interact with geographically diverse stakeholders including HCPs, KOLs, advisory boards, patients, payors, and internal/external audiences, but also present the challenges associated with communicating complex information without face-to-face interaction.
PERSONAL
The paradigm shift in the industry, requires MSLs to adapt their practices through specialized training including continuous learning for role proficiency, along with enhanced performance and career growth. The following considerations can guide organizations and individuals in their development of training programs and curricula. MSL training should be:
- Practical and able to be used immediately
- Tech-based, flexible & available 24/7
- Available in all formats
- Consumable as individual, low-commitment offerings but placed within a larger framework
- Collaborative and engaging, with learning enhanced by coaching and mentoring, games,accountability partnering, collaborative case study reviews, etc.
- With reduced burden of learning (cognitive load) to improve learners’ experience, for example bysimplifying messages, keeping trainings relevant to the role and accounting for time constraints.
Furthermore, trainings designed to help MSLs build the skillsets needed to keep pace with changing market, social, technological and regulatory conditions should include assessment and certification requirements, often including the following:
- Comprehensive certification, which includes disease area and product knowledge, communication skill, presentation skill, knowledge of relevant policies, compliance, and SOPs
- Modified manager certification based on field visits by manager to observe a Field Medical Professional interacting with Scientific Managers and Key Decision Makers
- Emerging assessment tools such as Axonify, an adaptive microlearning gaming experience that uses brain science techniques to build employee knowledge
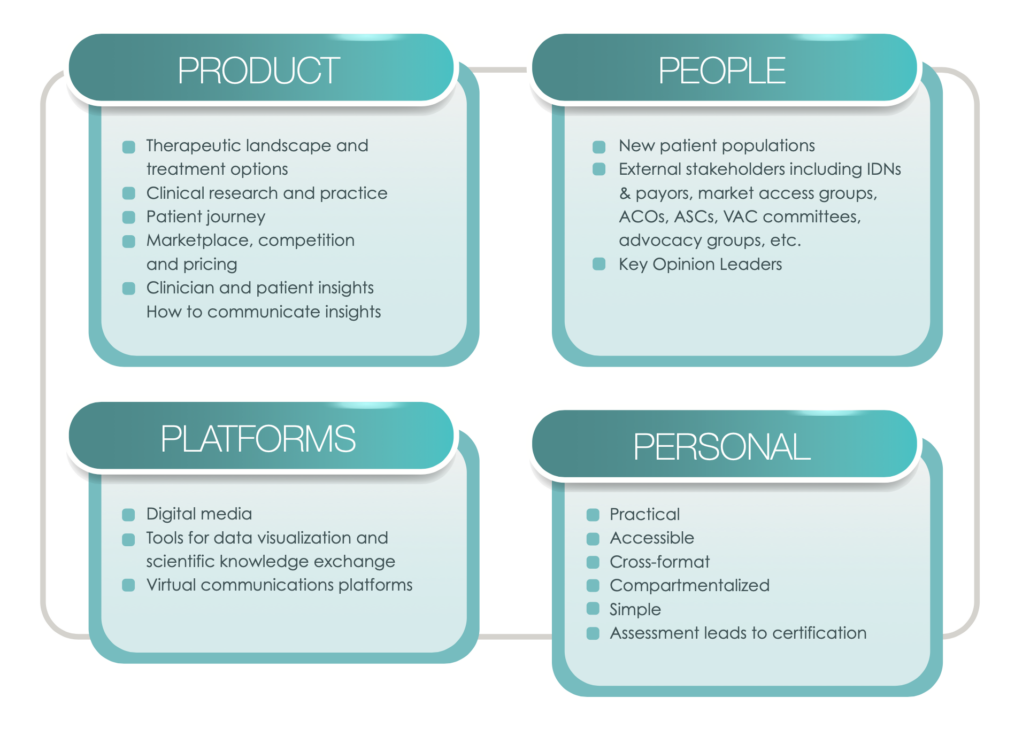
The Four 4 Ps: Considerations for MSL Training Design
SUMMARY
Innovations in science, data and digitization have transformed the healthcare landscape, leading to the emergence of new decision-makers and stakeholders. Alongside these innovations are shifts in culture and society that see patients playing a more active role in their treatments. These shifts are not hypothetical – they are here. The evolving healthcare environment presents both opportunity and challenge for MSLs to further differentiate their competencies, for example through specialized understanding of the therapeutic landscape, healthcare networks, and the requirements and desires of a diverse population of stakeholders. Through proactive engagement with new learnings, MSLs have the opportunity to broaden their vision, role and influence. These new skills will allow tomorrow’s MSLs to elevate performance across medical engagements to optimize experiences and outcomes for physicians and patients.
This publication represents the consensus opinions of the authors and various members of MAPS, but does not represent formal endorsement of conclusions by their organizations



