Authors

Emma Gough
Key Takeaways
- Anchoring content plans in HCP insights and building content for reuse reduces duplication and accelerates localisation. This should be supported by clear global vs local ownership to ensure assets are durable yet adaptable.
- Simple but effective personalised omnichannel interactions, with consent and compliance at the core, can deliver communications tailored to HCP needs while maximising impact.
- Closing the loop with performance indicators that prioritise learning over vanity metrics, focusing on asset adoption, outcomes, and impact while pruning outdated or low-value content, is essential to reduce content waste.
Introduction
Pharmaceutical companies produce a vast amount of medical and commercial materials every year. Medical education resources, field force decks, email campaigns, HCP portals, congress outputs and more are developed and often replicated at global, regional, and local levels. Yet much of this content never reaches its intended audience – in 2022, Veeva reported that 77% of content is either rarely or never used by field teams.1 At the same time, HCPs report being bombarded with information, with 55% of HCPs stating they feel overwhelmed with the content that is shared by pharmaceutical companies.2 This suggests that even when content does reach its audience, it can lack relevance, clarity and practical value. The result is a paradox: the potential to produce vast amounts of content, paired with diminishing returns on attention. Addressing this “content waste” is not simply a cost-saving exercise; it is central to effective scientific exchange and better patient outcomes.
What is Content Waste?
“Content waste” refers to any effort invested in planning, developing, reviewing, localising, distributing or storing materials that are not used or do not create discernible value for HCPs, patients or the business. Waste may manifest as global assets that never get adopted by affiliates, local adaptations that stall in review, emails opened but not read, decks shown once then archived, or congress outputs that generate little downstream education. It also comes at the cost of strengthening HCP relationships: MSLs lose time searching for materials and engagement with HCPs suffers from repetitive, misaligned messaging. So why does content waste persist? Organisational and cultural factors can reinforce each other. Global, regional and local teams often work to different timelines and priorities, leading to duplication. Content plans can be driven by internal events and calendars rather than HCP needs. Label and compliance variations create friction for reuse. Review processes encourage exhaustive completeness over clarity and usability. The net effect is a system optimised to make content, not to deliver impact.
How to Address Content Waste?
If we are to reverse this, there needs to be a shift to prioritise audience-centric value. HCPs don’t need more content; they need timely, credible and usable answers to specific clinical questions in formats that fit their workflow.
Start with insight, not format. Effective plans begin by understanding HCP need: what questions do they have at each point in the patient journey; what evidence do they trust; how do they prefer to learn; and what barriers stand between knowledge and clinical implementation? Together, advisory boards, qualitative interviews, field insight capture, congress listening and analytics from owned channels build a comprehensive profile of needs. These insight gathering activities should be ongoing, not a one-off exercise.
Prioritise fewer, better assets. Not every need identified warrants a new material. This can be tackled by implementing a simple gating mechanism: can we describe the audience, the need and the unique value of this asset vs existing materials, how it will be distributed, and how success will be measured? If these cannot be answered, it may be better to refine or repurpose an existing item.
Clarify global vs local roles. Content waste can proliferate when ownership is ambiguous. For example, it may be appropriate for global teams to own durable core components, overall strategic narratives and templates, with explicit guidance on what must remain unchanged and what is intended for local adaptation. Local insights, regulatory alignment and contextualisation may be better placed at an Affiliate level, with resources set aside for priority adaptations rather than spreading resource thinly across every asset.
Design for reuse from the outset. Reuse is not an afterthought; it should be a design choice. For example, modular content enables faster assembly of bespoke assets for different channels and markets. Crucially, “pre-localisation” considerations (e.g., where label differences are likely) should be captured in the global brief so affiliates can adapt with speed and confidence.
Make congress outputs work harder across the year. Congresses generate a wealth of data and discussion, but the value is often trapped in one-off assets. One way to tackle this is to plan a journey that has enduring impact: pre-congress context-setting that frames why sessions matter to your audience; live summaries that are fair, balanced and quick to digest; and post-congress materials that synthesise implications by specialty, regional relevance and practice setting. Capturing common questions, then prioritising follow-up content that directly answers them, can aid in maximising the value these materials bring. Where permitted, creation of affiliate-ready “local packs” with editable sections to incorporate local guidelines or label differences without rewriting the science can lead to efficient and consistent proliferation of content throughout markets.
Personalise omnichannel but keep it simple and compliant. Personalisation does not need to be complex to be effective. It starts with consented, preference-based communication and a pragmatic set of segments (for example, based on event attendance). Additionally, sequencing of interactions can be just as important as segmentation. For example, a congress poster might lead to a brief post-event summary for registrants who opted in; those who click through could be invited to a short webinar; attendees with unanswered questions might be routed to a follow-up one-to-one meeting. The same core content can be moulded into formats that match attention windows, such as a 90-second animation for a mechanism question, a one-page FAQ for dosing nuances, or a deeper interactive PDF for treatment guideline discussions. This allows HCPs to engage at the depth and time that suits them. All of these interactions must respect scientific exchange boundaries, local codes and privacy requirements.
Measure what matters and learn fast. Vanity metrics, such as counts of assets created and open rates in isolation, tell little about value. Instead, aim to track adoption and outcomes. At the global-local interface, this could mean the proportion of assets adapted and used by affiliates, and time to localisation. For HCP engagement, we should focus on signals of utility: completion of long-form content, follow-up requests, event attendance driven by content, and, where feasible, knowledge gained or self-reported intent to change practice.
Make change manageable. Shifting away from content waste is as much about people and incentives as it is about process. It is important to align goals so that teams are rewarded for reuse, adoption, and outcomes, not just output volume. This will help to shift the balance away from net-new production and towards insight generation, measurement and impact. Take the time to celebrate small wins: a module reused in ten markets; a post-congress summary email that doubled click-through rates by focusing on three practical takeaways in a bite sized format; a retired asset that was providing little value for the effort required to keep it updated and relevant – all of which are far more meaningful than producing yet another “new” piece of content that sees minimal engagement and ends up unused or discarded.
Shifting Mentality: From Wasteful to Impactful
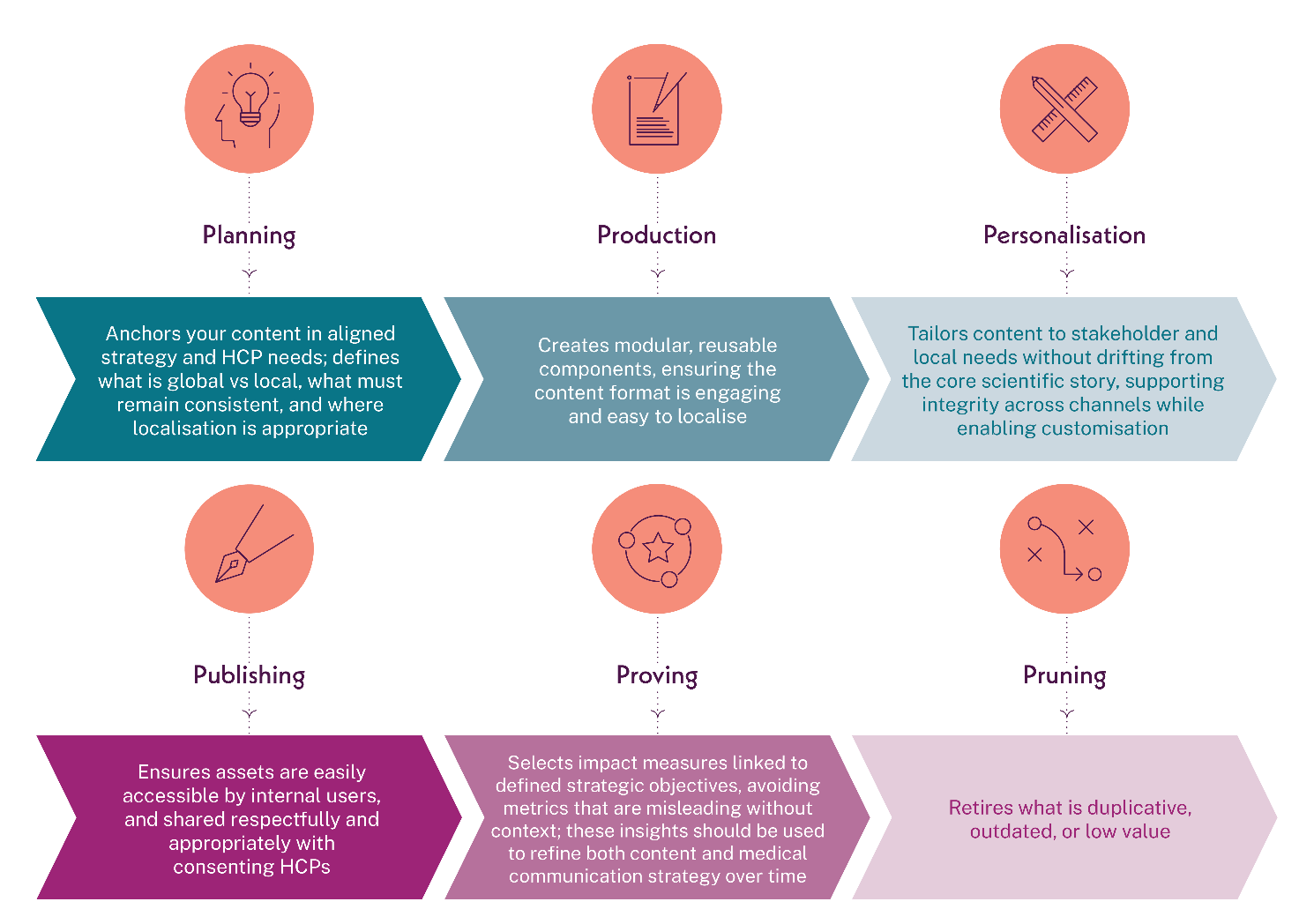
Tackling content waste starts with anchoring assets to strategy, for example using an integrated medical communications strategy that translates scientific narrative into a coordinated content plan across functions. Within that strategic backbone, teams can reduce waste through a simple lifecycle: plan, produce, personalise, publish, prove and prune.
- Planning: anchors your content in aligned strategy and HCP needs; defines what is global vs local, what must remain consistent, and where localisation is appropriate
- Production: creates modular, reusable components, ensuring the content format is engaging and easy to localise
- Personalisation: tailors content to stakeholder and local needs without drifting from the core scientific story, supporting integrity across channels while enabling customisation
- Publishing: ensures assets are easily accessible by internal users, and shared respectfully and appropriately with consenting HCPs
- Proving: selects impact measures linked to defined strategic objectives, avoiding metrics that are misleading without context; these insights should be used to refine both content and medical communication strategy over time
- Pruning: retires what is duplicative, outdated, or low value
Above all, we should resist the instinct to meet low engagement with more content. The scarcest resources are not budget or even time; they are HCP attention and trust. When Medical Affairs teams focus on creating fewer, better, reusable assets which are rooted in real needs, content stops being a production line and becomes a lever for impact. The payoff is practical: faster localisation, higher adoption, clearer scientific conversations, and a measurable reduction in noise.
Crucially, this shift is not just a vehicle for efficiency. As the scientific landscape becomes more complex and the volume of available data grows, clinicians face an increasingly overwhelming information burden. Industry analysis shows that tailored, data-driven medical engagement can help HCPs navigate this complexity more effectively and reduce suboptimal care by supporting more confident, evidence-based clinical choices.3 Elevating the clarity and strategic focus of content therefore has a direct line to patient impact, and strengthens the conditions for better-informed clinical choices where it matters most.
Note: The author used AI language-model assistance to draft and refine this article.
References:
- Veeva Pulse Field Trends Report Q4 2022 — https://www.veeva.com/resources/veeva-pulse-field-trends-report-4q22/
- Indegene Digitally-Savvy HCP Report — https://www.indegene.com/what-we-think/reports/digitally-savvy-hcp
- McKinsey & Company – A Vision for Medical Affairs 2030 — https://www.mckinsey.com/industries/life-sciences/our-insights/a-vision-for-medical-affairs-2030-five-priorities-for-patient-impact