Connect with Us
602 Park Point Drive, Suite 225, Golden, CO 80401 – +1 303.495.2073
© 2025 Medical Affairs Professional Society (MAPS). All Rights Reserved Worldwide.
Six in 10 Americans live with at least one chronic condition, with 33% reporting worsening symptoms during the pandemic, finds a recent survey of 2,627 people. Fatigue, depression and weight gain have all risen for people facing chronic conditions, and the fear of COVID-19 has drastically reduced in-person support from healthcare providers and even family. Despite this backdrop, and perhaps partly due to it, nearly a third of chronic disease patients are hesitant to get a COVID vaccine. Now is a critical time for Medical Affairs leaders to redefine their roles and boldly re-engage patients by employing a few key tactics learned from the past year.
As a Medical Affairs leader, one of the most important things you can do right now is listen to and internalize the toll the pandemic has taken on people living with a chronic health condition. What you’ll hear is striking.
These research findings shine a light on the fact that the pandemic has negatively impacted the underlying health of people already at risk. There is no time to waste in addressing the impending crisis poised to follow.


Consider how your Medical Affairs teams can support the following two patient engagement strategies:
1 – Provide Actionable Tips for At-Home Care
During Covid, many people turned to digital resources and online tools for help managing their health conditions. We expect this new habit to stick and see robust opportunities for building on new approaches that have proved effective. For example, the CDC reports a dramatic increase in the use of telemedicine, from 43% of health centers reporting the use of the telemedicine in 2019 to 95% using telemedicine during the pandemic.
Here at MyHealthTeams, we also see patients making use of online support communities both for connection and for health information and advice. One great example is the virtual pulmonary rehab offered to members of MyCOPDTeam, a social network for people diagnosed with chronic obstructive pulmonary disorder (COPD). The pandemic brought an abrupt halt to the pulmonary rehab sessions many people depend on, so we quickly teamed with the Home Rehabilitation Network, led by Alexander Grichuhin, to produce four videos that guide MyCOPDTeam members through techniques and tips they can use to strengthen breathing and maintain health at home. One example: a tutorial on pursed-lip breathing, which gently pressurizes the lungs and thus delivers more oxygen in any given breath.
The impact has been remarkable. When we surveyed members 30 days after the videos went live, we were thrilled to find that 92% of those who had seen the videos had tried the techniques – with 48% reporting they had done so more than 10 times.
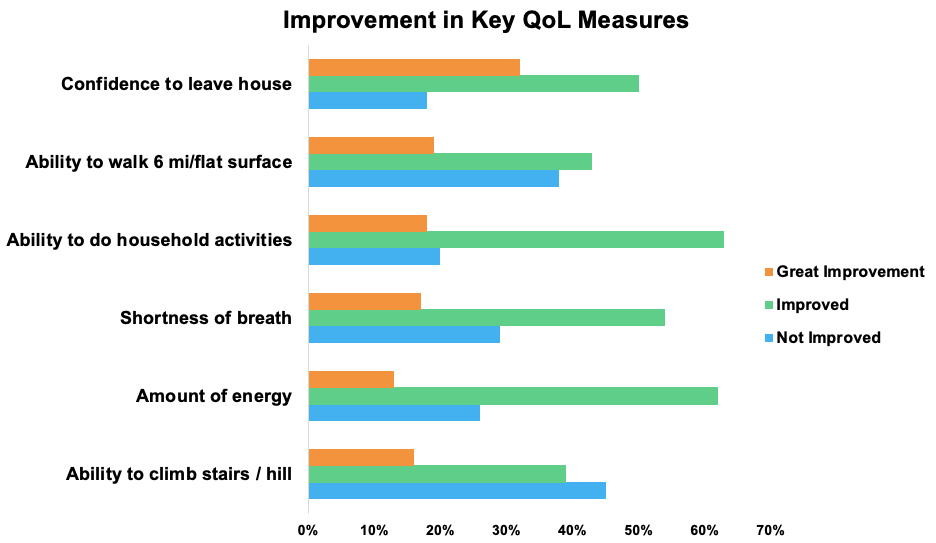
Then 90 days after the videos went live, we conducted a follow-up survey among a subset of the original respondents and found that 79% of them continued using the techniques regularly, which were associated with improvements in six key quality of life measures.
82% reported feeling more confident leaving their house and saw improvement in their ability to do household activities. Three quarters had more energy. 71% saw improvements in shortness of breath. 62% were more comfortable walking for 6 minutes on a flat surface. More than half were better able to climb stairs or a hill. This kind of impact is so valuable, enabling people to more effectively, comfortably, and safely do the things they want every day, at work and at home, for themselves and for their families.
Delivering health-promoting advice within the support system of an online community makes it easy for patients to adopt positive new habits that are realistic within the constraints of their daily lives – an essential step in helping to counteract the worsening symptoms of disease they have experienced over the past year. Medical Affairs leaders have the opportunity to accelerate this strategy, promoting the adoption of this virtual rehab approach in other therapeutic areas.
2 – Provide Condition-Specific Advice from Trusted Scientific Sources
36% of people with chronic conditions — the very conditions that put them at greater risk of severe cases of Covid — remain hesitant about, or downright resistant to, getting the COVID-19 vaccine. According to an ongoing study by Carnegie Melon University, this rate of vaccine hesitancy in the chronically ill population is more than half-again the rate of 23% found in the general population. Many people with chronic conditions report holding out because they want to hear directly from a doctor specializing in their disease that it is ok to get the vaccine. General guidelines from their clinic or from the CDC are not enough.
This presents a specific opportunity for Medical Affairs leadership, either in communicating this need for trusted guidance to healthcare providers or directly to patients, themselves.
For example, when one in three members of MyMSTeam — a social network for people with multiple sclerosis — said they were “waiting and seeing” before getting the vaccine, we invited Dr. Aaron Boster, a neurologist specializing in MS, to do a live Q&A on Zoom with members. More than 700 registrants submitted more than 300 questions in advance of the event. And thousands have since watched the video recording of the event.
In the course of one hour, Dr. Boster addressed the key concerns and questions raised by real MS patients regarding the COVID vaccine: potential flareup triggers, medication interference, and the cost/benefit of getting the vaccine. They heard an actual expert in their disease talk specifically about the vaccine and MS for the first time.
One hour later, it was astonishing to see the intentions of people change dramatically. The number of people who said they would “definitely get” the vaccine more than doubled — from 31% pre-event to 64% post-event. This kind of condition-specific patient education, delivered at scale, provides an actionable path forward for the chronic disease community and for all of us in the healthcare and biopharmaceutical industries trying to support them.
The pandemic has been challenging for all of us, and even more so for people living with chronic conditions. But the pandemic has also forced us to innovate new, sometimes better, ways of doing things — one example of which is new approaches to engaging patients. With new tools and new communities, we are listening to patients, working to understand their real-world experiences, addressing gaps in knowledge, and using this information to address gaps in care.
Medical Affairs leaders and the teams they oversee have a powerful role to play in this continuing evolution of patient engagement and education, providing trusted information and also meeting patients where they are to explore patients’ priorities and understand how we as an industry and as a society can meet these needs. Ultimately, our continued compassionate innovation will improve health outcomes by empowering people to make informed health decisions and take the actions that are right for them.


602 Park Point Drive, Suite 225, Golden, CO 80401 – +1 303.495.2073
© 2025 Medical Affairs Professional Society (MAPS). All Rights Reserved Worldwide.

 There is a magic when Medical and AI ethics are best friends
There is a magic when Medical and AI ethics are best friends