Connect with Us
602 Park Point Drive, Suite 225, Golden, CO 80401 – +1 303.495.2073
© 2024 Medical Affairs Professional Society (MAPS). All Rights Reserved Worldwide.

Pete Piliero, MD, moderates a discussion on contributions Medical Affairs makes to Asset Strategic Plans.
Medical Affairs thought leaders Q&A on topics including virtual congresses, digital platforms, and pre-print scientific publications.
Download the full article here
By
Ajit Patwardhan, MD1, MBA; Robin Winter-Sperry, MD2; Dannielle Heuer3; Stephen Valerio4; Urvashi Vashee5; Drilon Saliu, PharmD, MBA6; Greg Christopherson, PhD7; Irma Saliu, PharmD8; Kyle Kennedy9; Michelle Powell, PharmD10; Chris Brock, PharmD11 ; John B Pracyk, MD, PhD, MBA12; Joe Medicis, PharmD13
1 Physician – Surgeon, Medical Affairs Executive – Baxter International, Integra LifeSciences, NLT Spine, Paradigm Spine
2 President, Scientific Resilience; MAPS 2020 Co-Chair
3 Director WD Communications
4 Sr Director, Oncology Medical Training AstraZeneca
5 Global Scientific Training Merck & Co
6 Head, Global Medical Affairs, Clinical Development and HEOR, Connected Care Philips
7 VP, Medical Affairs Medline
8 National Director, Psychiatry MSLs, US Field Medical Allergan
9 VP, Customer Strategy – The Medical Affairs Company
10 Director, Filed Medical Excellence Astellas Medical Affairs Americas USA
11 Field Based Medical Affairs, Head, Respiratory GlaxoSmithKline
12 Integrated Leader, Medical Affairs, Pre-Clinical, & Clinical Research DePuy Synthes Spine, (J&J)
13 Director US Medical Affairs Callidiatas Therapeutics

The evolving role of Medical Sciences Liaisons (MSLs) was extensively discussed in multiple presentations and workshops at the March 2020 Medical Affairs Professional Society (MAPS) Global Annual Meeting in Miami, Florida. Executive leaders with domain expertise in building and managing Field Medical teams shared their experience and views on the value proposition of these roles and how a changing healthcare and industry landscape is influencing differentiation of and new opportunities for this role. The leaders also recognized the increased need for specialized training and how adult learning principles along with integration of new creative digital tools could help enhance engagement, performance and career growth. This article formalizes these learnings, providing best practices for MSLs in the context of the ongoing pandemic and beyond.
MSLs represent a core function of Medical Affairs, acting as the medical face of the organization to provide deep sub-specialty knowledge to healthcare providers and other external stakeholders. MSLs’ primary responsibility focuses on the three pillars of Medical Affairs, i.e. Scientific Exchange, Evidence Generation, and Evidence Dissemination. As such, a primary function of the MSL role is to build and execute an engagement plan in an expanding thought-leadership network. Currently, both the development of these plans and the actions that allow MSLs to deliver on their promise are undergoing sea change.
Over the last decade, healthcare delivery has undergone sweeping reforms. Emerging trends now focus on substantially better cost, quality, and outcomes as the new parameters to demonstrate significant healthcare value. Patients are now at the center of making their healthcare decisions and are demanding data transparency, easy/convenient access, and personalized products and services. Increased need for data transparency and availability has given rise to disruptive technologies and technological advances in the form of advanced data analytics, artificial intelligence, machine learning, digitization, new social media platforms, etc. Alongside these societal and cultural changes, stricter regulations and adjustments to healthcare policy (e.g. changing insurance landscape, use of Real World Evidence, new European Union (EU) regulations, increased scrutiny on drug pricing and rebates, etc.) are driving new ways of thought and action in the healthcare landscape. Meanwhile, the promise of new technologies driving basic and translational research have led Pharmaceuticals and MedTech industries to renew their focus on R&D and scientific advances, leading to personalized medicine breakthroughs in drug-device combinations, small molecule therapeutics, biologics, immunotherapy and diagnostic biomarkers, regenerative medicine and many more areas of advancement in the life sciences industry.
With these dynamic changes taking place in the healthcare landscape, the traditional role of an MSL as a bridge between internal company stakeholders and the outside medical community now needs to expand to encompass new competitive skillsets focusing broadly on Products, People, Personal & Platforms (“4Ps”). The following description of these 4Ps is not meant to be comprehensive, but rather is an attempt to start a new conversation about these core areas to better equip MSLs with a forward-looking understanding of the skill sets needed to succeed in the current and future disrupted healthcare landscape.
Due to increased need for personalized medicine (as described in part above), complex treatment options require deep therapeutic area expertise, which for MSLs includes the following:
The model of proscriptive medicine in which treatment decisions were made almost solely by healthcare providers has given way to a new model in which patients are collaborators or even drivers of treatment choices, often taking into account quality of life alongside quantity of life. This shift results in new stakeholders, including but certainly not limited to the following:
Along with new Products and new People are new Platforms that offer significant opportunity for MSLs to reach stakeholders with new creative digital tools for scientific engagement and education, including the following:
The paradigm shift in the industry, requires MSLs to adapt their practices through specialized training including continuous learning for role proficiency, along with enhanced performance and career growth. The following considerations can guide organizations and individuals in their development of training programs and curricula. MSL training should be:
Furthermore, trainings designed to help MSLs build the skillsets needed to keep pace with changing market, social, technological and regulatory conditions should include assessment and certification requirements, often including the following:
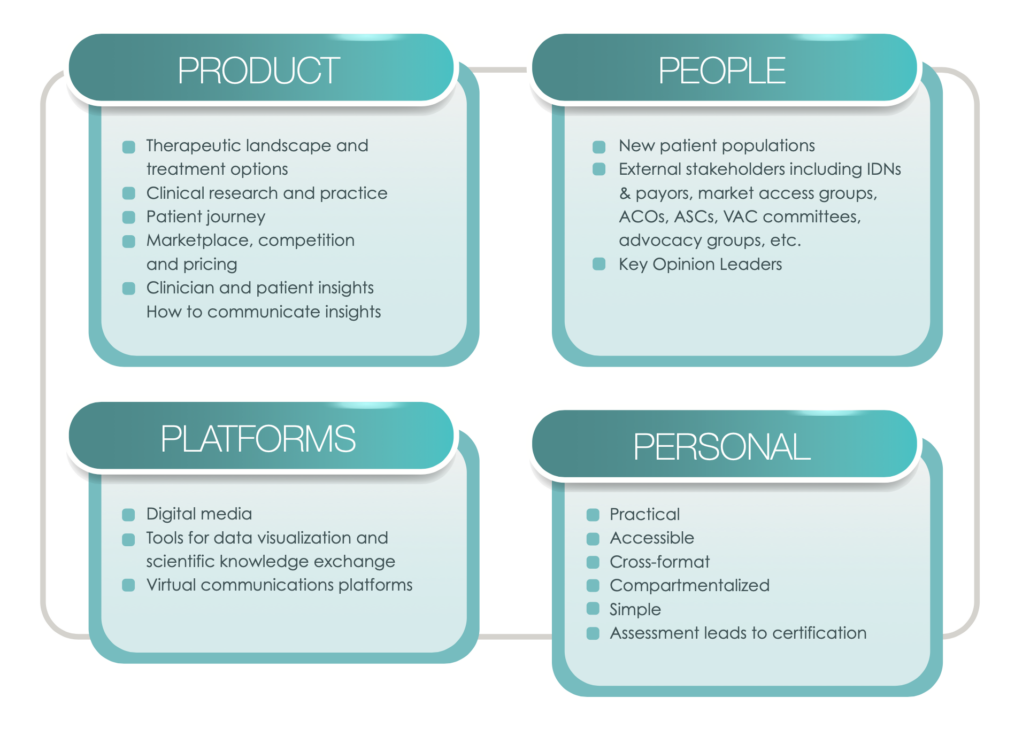
The Four 4 Ps: Considerations for MSL Training Design
Innovations in science, data and digitization have transformed the healthcare landscape, leading to the emergence of new decision-makers and stakeholders. Alongside these innovations are shifts in culture and society that see patients playing a more active role in their treatments. These shifts are not hypothetical – they are here. The evolving healthcare environment presents both opportunity and challenge for MSLs to further differentiate their competencies, for example through specialized understanding of the therapeutic landscape, healthcare networks, and the requirements and desires of a diverse population of stakeholders. Through proactive engagement with new learnings, MSLs have the opportunity to broaden their vision, role and influence. These new skills will allow tomorrow’s MSLs to elevate performance across medical engagements to optimize experiences and outcomes for physicians and patients.
This publication represents the consensus opinions of the authors and various members of MAPS, but does not represent formal endorsement of conclusions by their organizations
In July, Amgen’s Europe Medical Affairs team released results of a survey based on opinions of 441 healthcare providers (HCPs), detailing preferences for interactions with Medical Science Liaisons (MSLs) in light of COVID-19. Survey highlights include the following:
Here the Medical Affairs Professional Society (MAPS) speaks with Vice President of Amgen Europe Medical Affairs, Isma Benattia, about this survey and wider changes in the way MSLs work with their HCP peers during the pandemic and beyond.

Isma Benattia, MD, MBA, Vice President, Medical Affairs, Amgen Europe
MAPS: It seems like HCPs might have “pushed pause” on MSL interactions during the pandemic, but your survey shows almost the opposite, with majority of HCPs preferring fairly frequent interactions with MSLs. Did this surprise you?
Isma Benattia: We talk a lot about patient isolation, but we haven’t talked much about HCP isolation. Most of these physicians who don’t work in critical care were staying at home like everyone else. Among the very first interactions available were those with MSLs, using digital platforms, and I think it helped bring a sense of normalcy to physicians. Our survey results reflect the emotional experience as well. If HCPs want to maintain this frequent interaction, it means there must be some benefit in it for them – a need for this trusted interaction and source of information to take place.
MAPS: And you show the content of this need, as well, namely HCPs’ strong preference for scientific discussion and data.
Isma Benattia: The survey clearly indicated that physicians, even in the middle of this crisis, are always receptive to science and new information (not only related to COVID-19). MSLs play an important role in delivering this information. We are a source of innovation and scientific data. We are advancing the science together with the HCPs. It’s amazing how the collaboration efforts are happening. I see a great opportunity for MSLs to disseminate new knowledge and new science. After all, both the HCPs and the MSLs share the same objective – to serve patients.
MAPS: Of course, how MSLs disseminate knowledge is changing…
Isma Benattia: I was talking with a team member recently about digital strategy and he said: “It’s not a “digital strategy,” it’s the strategy for navigating in the digital world”. There is a big difference – not just equipping our teams with the right technology, but also being skilled and comfortable in communicating virtually. Technology is ready; I don’t think we’re as ready as the technology. The big challenge for us as an industry is not only to use digital platforms, but to adapt our content and its delivery appropriately. One cannot simply use a traditional slide deck! So, what other impactful channels can one use? That’s what MSLs need to learn to master.
MAPS: And how can MSLs go about this learning?
Isma Benattia: When I have a question or an issue, I call someone from our IT team – let’s call him “Bill”. That’s what MSLs need – their own “Bill”! A big part of the skills needed for digital transformation are different than the classical profile of an MSL. While I think technical training is important, you do not need to develop these skills; you can add (hire) these capabilities by adding new people who already possess the knowledge, working to support MSLs or, really, any of the Medical Affairs functions. Technology expertise doesn’t have to be a core competency for individual MSLs, but it needs to be a core capability for a Medical Affairs function. The combination of MSLs supported by new roles specializing in technology-based communication is absolutely fascinating.
MAPS: And Healthcare Providers, as well, have differing comfort levels with these technologies…
Isma Benattia: Yes, a video conference is very different from face-to-face interactions. I am also aware that some physicians in other regions of the world are eager to communicate via Whatsapp. I think we have an opportunity to make HCP interactions individualized, personalized, tailored experiences. For example, utilizing different HCP learning styles. We want to believe in the old model of slide decks and the idea that more information is better, but we need to understand individual HCP needs, preferences and expectations. One may be interested in reading an article, watching a short video, or listening to a podcast. I’m always amazed to see how much learning there is every day via all these channels.
MAPS: It sounds like you see a promising future.
Benattia: The digital model in general is a fantastic opportunity for our industry. Just look at the unprecedented attendance of virtual congresses! From a science dissemination point of view, what we can do digitally is just remarkable. Now you can get access to information when and how you want to absorb it. The question is what’s next.
MAPS: So…what’s next?
Isma Benattia: In my personal experience, even before COVID-19, I was trying to convince my teams that a multi-channel approach was the way to go and that we needed to start moving to a digital platform. Then everybody was forced to move 100% digital. And now, as you can see in this survey, HCPs see the future as a combination of the two – they’ve made this shift to a 50/50 model that combines face-to-face with virtual interactions. But we can’t forget that we’re still human beings and we like to see each other. It’s important to know the option of face-to-face still exists. I really doubt we will ever go back to pre-COVID-19 ways of doing things, but in the future, maybe this 50/50 model will be a standard.
MAPS: So, you see these changes as enduring, not just temporary adjustments?
Isma Benattia: Things are changing – our industry is changing – and the transformation is underway. COVID-19 acted as a catalyst for this transformation not just in HCP-MSL interactions and not just in Medical Affairs, but in the overall healthcare ecosystem. We saw this in our survey as well: HCPs now see virtual interactions and telehealth as essential pieces of the care delivery model. Patients like it, physicians like it – and it works. We also see a new appreciation for and emphasis on healthcare at a societal level. Before the pandemic, healthcare was deprioritized and this crisis shows that fundamentally health is a value that governments need to invest in, both on the preventive and also the therapeutic sides. In all these settings, MSLs have an important role as trusted sources of information on products, that connect internal and external interested parties. The challenge is and will continue to be about finding the balance between the traditional model of face-to-face interactions; in establishing a new model requiring competencies that mixes the traditional model with innovative, personalized, technology-driven ways to connect MSLs with HCPs in what is truly a new cultural, societal and healthcare landscape.
Download the full article here
By: Kirtida Pandya1, Jacqueline Waldrop2, Maria E. Vassilakis3, Marc Sirockman4, Deirdre Jordan5, Ogün Sazova6, Patricia Jassak7, Tim Mikhelashvili8, Sarah Funderburk9, Ivan Desviat10
In the Medical Affairs Professional Society (MAPS) community, external medical education can be categorized based on the extent of influence and industry involvement; however, it should always have the ultimate goal of optimizing patient care and improving health outcomes. Medical Affairs (MA) professionals take the lead to reach this goal by establishing external education programs to address knowledge, competency, or performance gaps. Educational strategies are implemented while fully complying with all applicable laws and codes and considering variables such as regional differences. External medical education demands are continuously evolving, and MA needs to continue to evolve with these changes to establish effective education strategies. Furthermore, the swift change to virtual education platforms due to the current COVID-19 pandemic requires speed and agility across stakeholders. The adaptation of medical education tactics will ensure effective healthcare professional (HCP) education, which will ultimately lead to improvement of patients’ healthcare.
The central mission of external medical education is to provide unbiased education to enhance healthcare professionals’ (HCP) knowledge, skills and competencies to improve patient outcomes. But what role do Medical Affairs (MA) professionals have in its creation and dissemination? The following article provides a brief overview of external medical education and gives insight into the integral role of MA professionals.
External medical education can be defined as diverse educational approaches provided to various stakeholders, such as HCPs, payers, patients, and caregivers, through education initiatives that aim to address identified knowledge, competency or performance gaps. Medical education may address therapy area and disease education gaps through scientific conferences, company-led education, continuing medical education (CME) grants and fellowships or diverse collaboration with scientific and patient advocacy societies (https://community.medicalaffairs.org/on-demand-conferences, The Role of Medical Affairs in External Medical Education: A Roadmap, Slide 11).
In its simplest terms, the primary goal that unites the entire industry across its MA functions is better patient care. In a systematic literature review of 39 studies, Marinopoulos et al. showed that independent medical education was indeed effective in improving the clinical outcomes of patients1. This was supported by Cervero and Gaines, who found that CME improves physician performance and clinical outcomes2.
MA professionals play a major role in the education needed to improve physician performance and patient outcomes. Based on their insights from diverse channels, they identify knowledge and competency gaps, and unmet medical needs. These can be addressed and translated into education for all stakeholders. MA professionals communicate and disseminate fair-balanced information that is important in guiding relevant strategies or tactics; however, their exact role varies depending on the level of independence of the approach and the extent of direct involvement, policies, and compliance requirements.
Independent medical education is supported through grant funding and is planned and implemented without the influence or control of the commercial supporter. Programs can be either funded through unsolicited grants, where third parties submit proposals, or through grants submitted in response to a Call for Grant Applications (CGA) or Request for Proposals (RFP). A wide variety of educational strategies are used at different lifecycle stages of a medicine or device. In the earlier stages it is crucial to assess the needs of healthcare providers and begin to close knowledge gaps, while the peri- and post-launch stages require predisposing, enabling and re-enforcing educational methods (Figure 1)3.
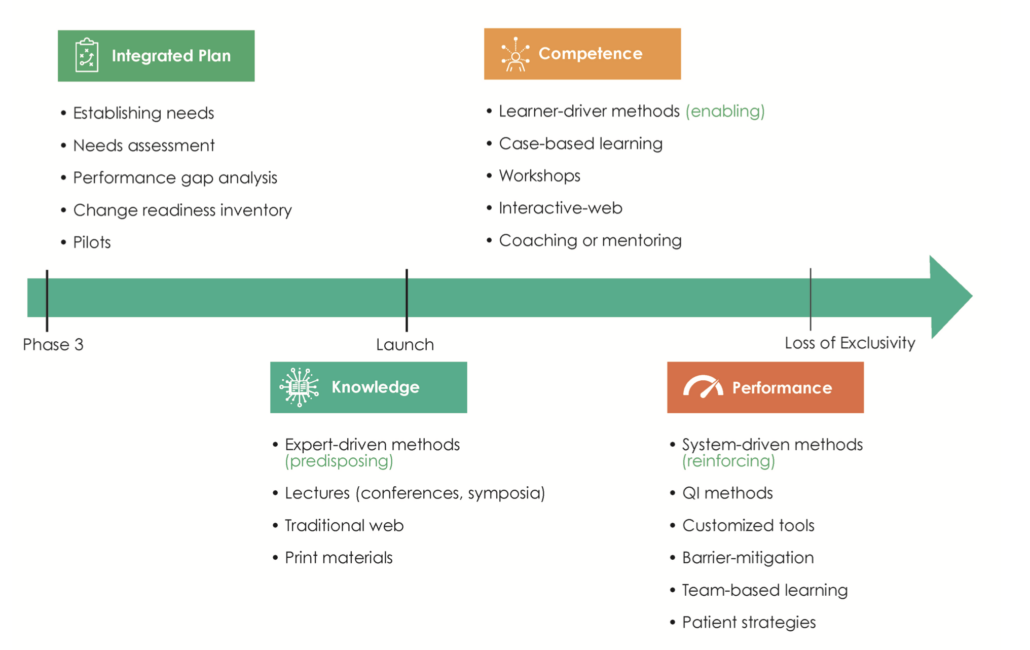
Figure 1. The planning of external medical education is aligned to the life cycle stages of a medicine. QI, Quality Improvement.
To strive for success, MA professionals are advised to keep the end goal in mind, thereby following a “backward planning” strategy. The final ideal state is identified first, then potential knowledge and competency gaps are identified, and finally, budget is allocated to a grantmaking strategy. MA professionals must also take into account the therapeutic landscape and other compounds/products in the specified area of interest.
Unsolicited independent medical education grants have historically utilized a reactive transaction where companies accept unsolicited proposals from accredited providers. MA professionals have had to change their approach to be able to proactively influence the healthcare landscape across a broad spectrum of stakeholders’ perspectives. Supporting needs assessment projects and extensive information-gathering must be used first to inform an effective independent medical education strategy, whether grants are submitted spontaneously or in response to a CGA or RFP.
Company-led medical education is another widely used form of external medical education. These activities are organized by individual pharmaceutical companies and might involve scientific committees, and/or independent scientific and professional organizations. Examples include scientific symposia, patient educational programs, company-sponsored meetings, and educational websites, among others.
Like independent medical education, company-led education is bound to the highest standards for quality, transparency and ethics in medical learning. Content must be relevant, credible, and timely, addressing educational gaps through a sound instructional design and outcome measure plan.
Regulatory agencies have diverse views on the classification of medical education developed by the pharmaceutical/biotech/device industry. Medical education and educational materials are rarely defined by their intent, but by the originator or the supporter. In this regard, industry-developed education/educational materials are considered promotional in many markets regardless of their nature and the internal function that develops them.
Medical education may play a role in influencing the market growth of therapeutics by increasing the awareness of disease states, treatments, and changing guidelines. However, the overall intent of medical education must not be to promote company products, devices, or solutions, but to improve HCPs’ knowledge of relevant data and integrate this into clinical competencies and skills which optimize patient outcomes.
It is important to note that various functions within the industry develop educational materials and scientific programs. While the medical education developed by the MA function does so in a scientific, non-promotional manner, there are components of education regularly developed or used by industry’s commercial function to complement their solutions with a primary intent to increase market share and sales of a product.
Legal and compliance implications in defining and implementing company-led education are extensive and are not addressed in this article. The MAPS Focus Area Working Group (FAWG) on External Education will be addressing these topics in an upcoming Standards and Guidance document and future e-Learning modules.
MA professionals need to measure the impact of educational initiatives on clinical practice and patient outcomes. Assessing relevance and effectiveness should be a continuous process throughout planning and implementation of an activity and needs assessment insights should inform the outcomes assessment plan. Activities should be continuously assessed for relevance and effectiveness and modified when needed. Moore and colleagues proposed a model of outcomes assessment that can aid MA professionals when evaluating activities for their impact on HCP performance and patient outcomes4.
To achieve positive outcomes for patients and healthcare systems, MA professionals need to be aware of potential hurdles they may encounter. Not only do they have the responsibility to ensure delivery of high-quality medical education externally, but they must also find a way to demonstrate the importance and positive impact of medical education to internal stakeholders. Furthermore, where previously physicians had the lead in making treatment decisions, due to rising healthcare costs, decision-making power is gradually shifting to a new set of stakeholders e.g., nurse practitioners and physician assistants who are helping to drive cost containment. It is crucial to be aware of regional differences affecting external medical education tactics (Figure 2). Variations in standard of care, availability of therapeutic products, and region-specific regulatory processes must be acknowledged when designing educational programs.
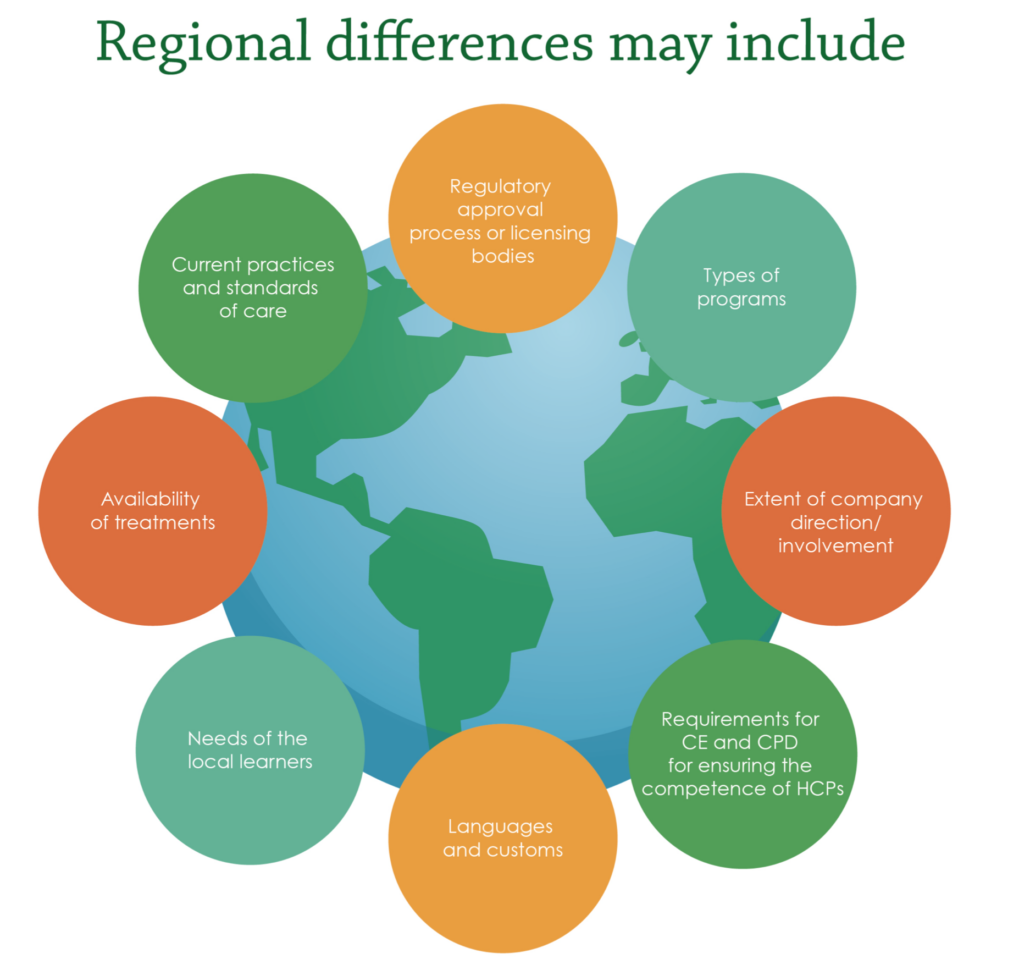
Figure 2. Regional differences in external medical education. CE, Continuing Education; CPD, Continuing Professional Development; HCPs, Healthcare Professionals.
External medical education is rapidly evolving, and MA professionals must be ready for swift changes. Healthcare scientific data continue to increase and originate from an ever-expanding range of sources such as real-world evidence and social-listening programs. The need for external education supporting HCPs as they decipher and incorporate this information requires adaptive education strategies. Medical education is part of HCPs’ lifelong professional development and must address learning needs most relevant to their daily practice5. Increasing transparency in the industry requires data generation and dissemination around external medical education programs, particularly transfers of value (TOV) to HCPs. Additionally, patient advocacy groups are more frequently included in decision-making, maximizing patient insights and directing education strategies towards a more patient-oriented approach.
The recent rapid transition to virtual learning has enhanced disseminating educational content during the ongoing COVID-19 pandemic. MA professionals must adapt to challenging times and find new, diverse ways to generate, and disseminate educational content effectively to support HCPs’ and patients’ needs. A “one size fits all” approach is inadequate for virtual content when delivering medical education in the current situation. A tailored, agile approach aligned to the appropriate setting and audience will allow MA professionals to provide successful digital education and establish the most suitable forum within which to improve timely data dissemination. The right information and education delivered in the appropriate format to HCPs will translate into enhanced and more effective patient care, ultimately improving patient health outcomes.
MA professionals are uniquely positioned to serve as factual, impartial, trusted partners who align company strategy to meet healthcare stakeholders’ and patients’ needs. They lead implementation and support of external education with the goal of improving patient outcomes. Gathering internal and external stakeholder insights while keeping the end goal in mind will transform the ever-changing relevance and value of MA strategy and tactics. Thus, as the field of external medical education evolves, MA professionals must adapt accordingly by keeping abreast of the latest healthcare institutional system changes, regulatory codes and compliance needs, regional differences, and technology advances. This will ensure that our key stakeholders (HCPs) have access to quality, evidence-based scientific data to address education gaps to optimize patient care and impact health outcomes.



Scientific communication platforms have rapidly evolved to serve as the foundation of a consistent and effective cross-functional Medical Affairs communication plan. These platforms are a necessary tool in the arsenal of all Medical Affairs professionals, and the MAPS Standards and Guidance document provides clarity on developing and implementing scientific platforms for all Medical Affairs professionals, ranging from novice to expert.

At the end of the webinar participants will have a better understanding of:
• What is company and medical affairs lead education and how it is perceived by audience
• What are the different perspectives existing among regulators, Pharma and agencies
• The potential for disease state medical education by medical affairs

602 Park Point Drive, Suite 225, Golden, CO 80401 – +1 303.495.2073
© 2024 Medical Affairs Professional Society (MAPS). All Rights Reserved Worldwide.
