Connect with Us
602 Park Point Drive, Suite 225, Golden, CO 80401 – +1 303.495.2073
© 2024 Medical Affairs Professional Society (MAPS). All Rights Reserved Worldwide.

Medical Affairs (MA) teams demonstrate leadership and value through the annual strategic planning process. The medical plan serves as a roadmap clearly communicating the core medical strategy and supporting tactics, aligning all multifunctional MA competencies and geographies on common objectives. These objectives support the product and organization, and depend on a focused, cohesive, and aligned medical strategy. The strategy is the foundation for the year ahead and will serve as guidance for overcoming challenges, taking advantages of opportunities, and filling any scientific or clinical gaps. This webinar is an introduction to strategic planning principles that can be employed to develop a successful medical plan.
After completing in this webinar, participants will be able to:
• Understand the value of having a thoughtful Medical plan
• Identify critical success factors and potential pitfalls in developing a strategic Medical plan
• Work with the MAPS Standards and Guidance Medical Affairs Strategic Plan template and guide
The digital health revolution implies a clear understanding of strategy, using technology as an enabler to create better outcomes for patients and to power value creation across the healthcare ecosystem. As data specialists, Medical Affairs professionals will be at the forefront of this transformation.
 The medical world is changing and changing fast. As multiple new technologies start to transform every aspect of the healthcare ecosystem and the lines between biosciences and data science fade, companies need medical leaders who not only understand the latest medical advances but also the potential and scope of data and digital, along with their implications – not least that this new paradigm requires strategists who are comfortable with organizational transformation and who can lead change. Dr Rajni Aneja is one such strategist: she specializes in the crossover between business and technology across a variety of health sectors.
The medical world is changing and changing fast. As multiple new technologies start to transform every aspect of the healthcare ecosystem and the lines between biosciences and data science fade, companies need medical leaders who not only understand the latest medical advances but also the potential and scope of data and digital, along with their implications – not least that this new paradigm requires strategists who are comfortable with organizational transformation and who can lead change. Dr Rajni Aneja is one such strategist: she specializes in the crossover between business and technology across a variety of health sectors.
“My training falls at the intersection of business and technology and I have worked across all different healthcare sectors from payer to a consumer digital company to pharma, as well as being involved in an advisory capacity for innovation and strategy in health for MIT and Harvard Innovation Lab, along with Oliver Wyman, and many other start-up companies.
“From an industry standpoint, I am interested in the role of digital facilitating consumer as well as HCP engagement strategies, or patient journeys through a variety of touch points leading to better clinical outcomes, better clinical interactions, better patient experiences, better healthcare provider experiences, as well as better delivery of healthcare.”
This approach is all about strategically using digital as an enabler driven by data. “When we create a strategy around a digital experience, it’s not about the technology. I see the technology as an enabler: when you apply the right technology at the right point and have the right interventions designed – either for the provider or patients – that is when it actually is impactful or meaningful.”
Longer term, advances in bioscience and digital technology have the potential to add value to the system in multiple ways: for example, by transforming the R&D process to potentially make it shorter, more specific, and take out cost; by ensuring better health outcomes for patients, bringing forward new treatments more quickly, and generally improving the patient experience; and by providing opportunities for physicians through new options to advance patient care and offering new ways to engage and learn.
We are only at the start of this journey today but Dr Aneja points to significant potential that already exists. “As a physician, when you see patients in clinics, you’re only seeing 15 to 20 patients in a day. But if you have technologies like telemedicine, where you are delivering consultations on videos, or you’re delivering care to remote areas, your impact and outreach becomes much wider and much more significant.
“I see telemedicine as one of the technologies to have gained a lot of momentum, not only for its potential in clinical trials but also for prevention and wellness visits, or even acute care visits. But what’s coming next? I think the future is where data is driving or enabling these technologies, and this is where artificial intelligence or machine learning comes into play. However, if the data is not good enough, anything that is going to come out of it is not going to be good enough: garbage in, garbage out. The importance of data as an asset is that you drive intelligent decision-making and that is only done through insights generated by the power of data that is collected from a variety of technology enablers.” As an example, she cites finding the right patient for the right clinical trial at the right time for the right medical condition, while delivering the right care, all of which can be powered and informed by the data.
Today, real-world evidence (RWE) and data – especially continuous real-time data – sits at the heart of where the healthcare ecosystem is headed, not least in the context of value-based health design and care delivery, where (especially in the US) the system is moving from volume to value, and there is more emphasis on better outcomes. This implies that data can be both shared and combined effectively, and also that RWE – including data directly from the consumer, say from wearables – can be integrated with historical data and combined with real-time analytics.
“There’s an evolving trend that we’re seeing: in the last two to three years pharmaceutical companies have started to work very closely with the payers. But the industry is becoming disrupted and I think all these stakeholders can learn from each other to say: ‘How am I going to be a leader in the game instead of a follower?’”
The trend within the healthcare sector is asking for more integration of data and collaboration between organizations – joining the dots – to generate insight from the payers as well as from pharma and from consumers. “This is a collaborative effort around value-based care and an outcome-based approach, which will lead to better patient care and better clinical trials. But there are many challenges remaining before this data utopia becomes reality, including a lack of agreement on definitions of what constitutes value. What is considered good-quality data, data privacy, data governance and data security and many others factors would play a vital role in shaping the thought process as we move along this transformation journey.”

So, what are the hurdles? The regulatory environment is one, but regulators and government are increasingly aware of the need to advance. We have seen the introduction of the 21st Century Cures Act; as well as statement from FDA commissioner, Scott Gottlieb about the importance of digital health and real-world evidence, and there are efforts now around guidance from the governing bodies. Commercial sensitivity is another issue, but industry is increasingly acknowledging the need for collaboration – perhaps through neutral consortium – to harness the power of data and analytics. As an example, Dr Aneja cites the NEWDIGS project, through MIT’s Center of Biomedical Innovation, which brought together various pharmaceutical partners in a neutral, non-biased, cohesive setting. However, she acknowledges that “we’re taking baby steps and are in exploration mode with a desire for more collaborative models, and not yet ready for prime time yet.”
 And what about the benefits? There is clearly substantial value in a system that encourages us to learn about the patient – not least, greater customization, personalization, and simplicity for the patient. This encompasses patient-reported outcomes, behavioral profiles, social, and other demographic data leading to consumer segmentation, which in turn can deliver on targeted interventions and interactions.
And what about the benefits? There is clearly substantial value in a system that encourages us to learn about the patient – not least, greater customization, personalization, and simplicity for the patient. This encompasses patient-reported outcomes, behavioral profiles, social, and other demographic data leading to consumer segmentation, which in turn can deliver on targeted interventions and interactions.
Dr Aneja elaborates: “I’ll give you an example. Rajni is a 40-year-old female who runs every day and is pretty healthy and motivated and doesn’t take any medicine, but is very interested in her well-being. Because of the combination of data from different sources, we can create a profile of what Rajni wants, what Rajni needs, how we engage her, how we motivate her and do that on a continuous long-term basis; and data can enable targeted, personalized interventions – interactions that are actually applicable to Rajni, not one-size-fits-all. Data can help you get to that level of granularity, but I always say that with a word of caution: we’re not there yet. But that doesn’t mean that we can’t get there; it’s just that we’re on our way to this kind of transformation.”
And this opens up a whole world of further possibilities: Rajni might be part of a cohort that you could segment in the context of preventative health and screening, and so on. So there’s an opportunity to gain a depth of insight into individual patients within a population. “Imagine if you could understand, in your population, who are my well people? Who are my sick people? Who are the people who are very, very motivated? Who are people that actually need a lot of nudging because they’re not motivated? With the years of data, you have the ability to be not only predictive but at some point can be prescriptive, especially for precision medicine.”
Beyond this, digital needs to make life simpler and more convenient for patients. Healthcare is already becoming more consumer-centric. “I think it’s already happening. You already have Uber Health; we have telemedicine solutions; we have remote monitoring; we have wearables and sensors. I think the trend that we see is consumers becoming more involved in taking responsibility for health; they’re becoming more informed. Consumers want to manage their health, want to see their healthcare data, and want to be equally responsible for decision-making.

What needs to happen going forward? “I think it’s an industry shift.” There is recognition that we need to accelerate this process, according to Dr Aneja. In conclusion, she sees a significant role for Medical Affairs within this new environment – as the conduit of the digital transformation. MA can help define the problems we are trying to solve, along with the data sets and technology that will enable a solution. “They are absolutely vital. You would not create an initiative in a silo; technology is an enabler. Ultimately the insights coming from MA about what problems we need to create an effective solution for will lead to better patient outcomes as well as better patient experience.”
Biography
Rajni Aneja is an MIT Connection Science Fellow, healthcare strategist, public speaker, and transformative change agent with expertise in population health management and digital health. She serves as an adviser to a variety of health and wellness organizations. Dr Aneja encompasses various vantage points as a clinician, executive, adviser, entrepreneur, speaker and technology advocate serving in senior leadership roles. These include Chief Medical Officer for WebMD health, EVP of Joslin and a strategic executive and transformation leader at Humana. Most recently she contributed to the building of a digital consumer strategy at Novartis. Dr Aneja received her MD from Research Medical Center in Kansas City and her MBA from the University of Massachusetts.
Medical Affairs leaders want to be more effective and valuable. They want to secure their seat at the table and influence decisions, impact company performance, and deliver better patient outcomes. To do this, they need to understand the “big picture” of the business and grasp how their decisions and actions contribute to long-term profitability and growth. Or in other words, MA leaders need strong business acumen.
 Many MA leaders, though functionally brilliant, may not count business acumen as a core skill. But they are not alone. Harvard Business Review confirms that 95% of employees do not fully understand their company’s strategy. “This is not an indictment of Medical Affairs leaders, by the way,” says Ben Cook, President of Acumen Learning, a training organization that specializes in business acumen training and counts 23 of the Fortune 50 among its client list. “Pretty much every function is represented in that data point. But the net effect across the board is the same. I like to compare it to a commercial I recently saw – there’s a guy in a suit diligently clearing and scraping snow from his car but then he discovers that it’s not actually his car. MA can likewise focus too much on their function and technical expertise, only to find themselves expending energy in ways that are not aligned with the company’s objectives.”
Many MA leaders, though functionally brilliant, may not count business acumen as a core skill. But they are not alone. Harvard Business Review confirms that 95% of employees do not fully understand their company’s strategy. “This is not an indictment of Medical Affairs leaders, by the way,” says Ben Cook, President of Acumen Learning, a training organization that specializes in business acumen training and counts 23 of the Fortune 50 among its client list. “Pretty much every function is represented in that data point. But the net effect across the board is the same. I like to compare it to a commercial I recently saw – there’s a guy in a suit diligently clearing and scraping snow from his car but then he discovers that it’s not actually his car. MA can likewise focus too much on their function and technical expertise, only to find themselves expending energy in ways that are not aligned with the company’s objectives.”
According to Cook, MA speaks the language of Medical Affairs fluently, but they lack the business acumen needed to speak the language of business. This inability to speak the same language as the C-suite is hampering MA’s influence. “If you are making a recommendation but you’re not speaking the language of the executive team, it’s not fitting with where they’re trying to go, so the ability to gain access to resources in order to fulfill that vision is certainly not going to be there in most cases. So, we have to align our priorities and focus on areas that the executive team, who sign off on these decisions, are most attentive to. Our credibility, our access to resources, and our ability to partner is best enabled when we understand where the company is going. We need to start asking, ‘Are we scraping the right windows?’”

Another driver for MA to build its business acumen muscle is the growing requirement for MA professionals to interact with C-suite executives from health systems and health plans as well as other decision-makers who are responsible for market access and formulary decisions. Effectively playing these roles will likely require different skills and competencies that have not traditionally been central to the MA function. “The circle of medicine development, licensing, reimbursement and commercialization requires the creation of value for all stakeholders and being focused on sustainable value generation is thus a must for Medical Affairs professionals who play a pivotal role in all aspects of this circle,” says Michael Zaiac, Head of Medical Affairs Oncology, Region Europe, Novartis.
Armed with business acumen, MA can operate a number of levers both internally and externally to drive value. “Internally, MA can deliver integrated insights efficiently and inform development programs accurately, allowing for optimized development plans yielding reimbursable medicines. People with business acumen are more aware of operational efficiencies, as they understand the way different contributions affect the different elements. Any imbalances here are inefficient. Externally, MA can support the development of novel business cases or beyond-the-pill services that greatly enhance the value of a medicine to all stakeholders, which often makes the difference to patients having or not having access to critical medicines. Business acumen is key to identifying the most sustainable and successful ways for value generation for patients through identifying the right stakeholders and addressing their needs,” says Zaiac.
For Cook, the time has come to re-examine the role and level of influence of Medical Affairs in a world focused on communicating the economic and health system value of a product, rather than “selling”. “Medical Affairs is often thought of as a cost center but there are a number of ways MA can really drive value. Communicating treatment value using scientific and medical information in a manner that supports the incentives and needs of the various stakeholder groups is one way, but it requires an appreciation of hospital and IDN (Integrated Delivery Network) incentives and the long-term strategic imperatives at play. The ability to link arm in arm to find mutual incentives that drive health outcomes can actually have a huge impact on a global basis.”
Operational efficiency isn’t a sexy concept, but it is the key to fully maximizing profit and boosting the bottom line. Senior leaders can’t afford to work in silos and behave as independent functional experts. In today’s dynamic environment, both cross-disciplinary collaboration and deep functional expertise are required skills. Medical Affairs must look at how it can cultivate the ability to anticipate needs among a much broader range of stakeholders to deliver value for both patients and the healthcare ecosystem through the delivery of superior medical outcomes, while simultaneously reining in costs and reducing excessive spending.
“There’s an old adage that says a dollar saved is a dollar earned, but that’s not the complete story. Imagine you’re able to save $100 (Option B), that $100 will drop straight to your bottom line less any additional expenses like taxes. If taxes are 20%, that would leave you with $80 in additional profit. Now let’s say that you’re able to increase revenues by $100 through selling additional products (Option A), a lot of that additional revenue will be eaten by the cost of creating and selling those products. If those costs are $80, that would leave you with $20 in additional profit. If you can be a little more attentive to Option B, you have four times the impact on the bottom line. This is a simple concept, but it’s one that most people don’t think about.”
For Cook, there’s a real opportunity to build credibility and free up resources to spend in other areas. “If Medical Affairs can understand these levers and appreciate both sides, they’re seeing the big picture. If you can develop your Option B mindset and use the language of Option B in your business cases, you’ll start to elevate your credibility especially with those who already have this mindset, like finance. That’s not to say that I’m favoring one lever over the other; we all know that if you push too hard on driving efficiencies, you can hamper growth, or negatively impact people. You have to be considerate of the five drivers of business: cash, profit, assets, growth, and people. When you’re able to balance these drivers, you’re helping the business run better, which enables the company to create more lifesaving products.”
Today’s industry also faces considerable headwinds. The outlook for pricing and volume expansion is becoming less attractive across all regions, given the sustained pressure on drug pricing in Europe, the growing size and bargaining power of payors in the United States, the looming biologics patent cliff, and the mounting competitive pressure in emerging markets. Meanwhile, advances in technology and analytics are opening up opportunities for powerful tech entrants to engage with patients and consumers in radically new ways, offering innovative healthcare solutions in conjunction with payors and providers. These entrants threaten to disintermediate pharma companies as the primary owners of patient data and take control of their value story. Should that happen, it would have drastic repercussions for pharma’s R&D and commercial models.1
Why UPS trucks (almost) never turn left
In a challenging business environment, operational efficiency and cost control become increasingly important. Cook illustrated this point with a story from UPS: “By keeping left-hand turns to a minimum, UPS saves millions of dollars in fuel and reduces CO2 emissions by more than 100,000 metric tonnes a year. This seemingly simple idea has a $100 million impact to the bottom line each quarter. Now that’s impact! We need to start asking, ‘What right turns can we make in Medical Affairs to demonstrate our value?’”
Historically, companies have narrowly defined the role of Medical Affairs, but if you want to be more visible and valued, you need to demonstrate your business acumen and how MA fits into the big picture of the overall business. “As we think about growing our market share, we need also to think about the most efficient ways to get there and how to marshal the resources we already have to optimize our impact. Remember, you can be functionally brilliant, but unless you see that big picture and develop your business acumen, you’ll have very little influence with senior leader decision-makers. In other words, your ideas and proposals will have less of an impact.”
Sources:
1: Rethinking Pharma Productivity https://www.mckinsey.com/industries/pharmaceuticals-and-medical-products/our-insights/rethinking-pharma-productivity
Business acumen is keen, fundamental, street-smart insight into how your business operates and how it makes money and sustains profitable growth, now and in the future. Understanding the “business of the business” is critical to know which opportunities to pursue and which to ignore.
Benefits for Medical Affairs:
Armed with business acumen, Medical Affairs leaders can influence top-line revenue and bottom-line profitability, and prioritize day-to-day actions in alignment with organizational strategy. The result? More resourcing, more credibility, better partnership.
Five Business Drivers:
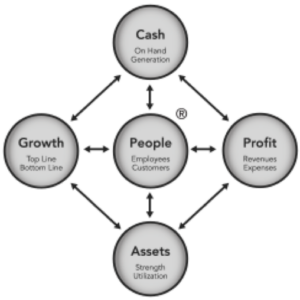
Cash – Cash is the fuel that drives a business; it’s more important than your mother as the founder of Seagate Technology once said. Without cash, a business can’t pay its bills, can’t pay its employees, can’t buy the goods it needs to produce the products or services it sells. If you evaluate the three key components of cash – cash position, cash flow, and liquidity – you will have a better understanding of how you generate cash and how to use it wisely and spur growth. Pharmaceutical and Medical Device companies actually need significantly more cash than the average company due to the risk and time required for developing products, getting those products to market, making acquisitions/buying licenses/trademarks/patents, and supporting the development of future products.
Profit – Profit is simply the difference between how much you make by selling goods and services and how much it costs to produce and sell them. By looking at the differences between profit and cash flow, and explore the concept of profit margin, you can reveal how efficiently a company is turning revenue into profit. Pharmaceutical and medical device companies typically have higher profit margins than the average company to compensate for the higher risk in developing products that need to pass regulatory approvals and gain market access, and the extended time the companies spent on product development, the regulatory processes, the market-access process, and support in getting products to market.
Assets – Assets include everything a company uses to produce revenue, whether these are tangible, such as buildings and equipment, or intangible, such as patents. Balancing asset strength with asset utilization is a dilemma all businesses face; having more resources to buffer the company from uncertainty is beneficial but making sure any asset the company has is most optimally deployed is also a vital priority for successful companies. Exploring how a company meets its obligations, takes advantage of opportunities and survives tough economic times – with asset utilization – is vital to produce revenue and sustainable growth. Many drug and medical companies could benefit from enhanced scrutiny on its processes and systems to ensure they are most efficient and are eliminating waste and non-value-added activities.
Growth – Constant change is a reality in today’s business environment, and growth is one of the few ways to handle it. Growth can be measured in terms of both revenue and profit. Understanding how growth strategies impact business performance and the bottom line will provide a smoother roadmap to success. Making sure the company is able to grow its top-line faster than the market through innovation, differentiation, market development, and speed is vital. But companies also need to ensure their bottom line is also growing as they operate as efficiently as possible to ensure sales translate into profits.
People – People lie at the center of the five key drivers. Kevin Cope, founder of Acumen Learning says: “People make the decisions, supply the financial resources, buy the products, and provide the labor and services. They drive cash, profit, assets, and growth. Meeting, exceeding, and even anticipating the wants, needs, and expectations of your employees, customers, and other important stakeholders is essential to your financial success.” And with Medical Affairs sitting at the vital nexus of R&D, Commercial, and customers, it is extremely vital for MA to understand what each part needs and wants and how to best deliver those in the best way possible.
Source: Acumen Learning
1. MSL deployment – marshal resources at the right time to optimize resources and minimize cost.
2. Digital transformation – streamline costbase to improve internal or external customer experience.
3. Process engineering – look at every process that is less efficient than it needs to be and drive improvements in those processes.
4. Tight collaboration – while working with the other functions, collaborate tightly to ensure limited duplication of activities, limit rework due to miscommunication, and find clear agreement early on to the goals/outcomes for initiatives to accomplish well-defined roadmaps.
5. Organizational knowledge transfer – not only collaboration across functions and geographies, but also capture and make accessible key learnings at all levels with initiatives to ensure mistakes don’t proliferate and key learnings are institutionalized.

Understand the latest technologies—Artificial Intelligence (AI), Machine Learning (ML), Natural Language Processing (NLP), and Natural Language Understanding (NLU). Understand the potential of these technologies to increase efficiencies, enhance effectiveness and potentially reduce compliance risk.
At the conclusion of this session, participants should:
• Better understand contemporary digital trends of Artificial Intelligence (AI), Machine Learning (ML), Natural Language Processing (NLP), and Natural Language Understanding (NLU)
602 Park Point Drive, Suite 225, Golden, CO 80401 – +1 303.495.2073
© 2024 Medical Affairs Professional Society (MAPS). All Rights Reserved Worldwide.
